In this guide, you’ll discover 7 powerful signs that your struggles may be rooted in unprocessed trauma, what trauma-informed care actually looks like, and where Portsmouth and Hampton Roads residents can access compassionate, evidence-based treatment right now.
You’ve been told to “just move on.” Maybe you’ve even told yourself the same thing — that it wasn’t that bad, that others have been through worse, that you should be over it by now.
But your body hasn’t gotten the memo.
You’re exhausted in ways sleep doesn’t fix. You feel on edge without knowing why. Relationships that should feel safe still feel like minefields. And somewhere deep down, you’ve started to wonder if this is just who you are now — if the version of you from before is simply gone.
It isn’t. And you are not broken.
According to SAMHSA, more than 70% of adults in the United States have experienced at least one traumatic event in their lifetime. What most people don’t realize is that trauma doesn’t just live in your memories — it lives in your nervous system, your body, and your daily behaviors. Standard care often misses this entirely. Trauma-informed care doesn’t.
Quick Answer: What Is Trauma-Informed Care?
Trauma-informed care is a clinical approach that recognizes the widespread impact of trauma on the brain, body, and behavior. Rather than asking “What is wrong with you?”, trauma-informed providers ask “What happened to you?” — creating a safe, empowering environment built on trust, collaboration, and the understanding that trauma responses are not character flaws. They are survival adaptations.
Table of Contents
- What Is Trauma-Informed Care? (And Why It’s Different)
- 7 Powerful Signs You May Need Trauma-Informed Care
- What Makes Trauma-Informed Care Different from Regular Therapy?
- Finding Trauma-Informed Care in Portsmouth, VA
- Frequently Asked Questions
What Is Trauma-Informed Care? (And Why It’s Different)
Trauma-informed care (TIC) is not a single treatment technique. It is a foundational framework — a lens through which every interaction, every question, and every clinical decision is made with the awareness that trauma may be shaping your experience right now, in this room.
Traditional mental health care often treats symptoms in isolation: anxiety is medicated, depression is processed, insomnia is managed. Trauma-informed care goes further. It treats the root — the disrupted nervous system, the fractured sense of safety, the survival patterns that once protected you but now hold you back.
The 5 Core Principles of Trauma-Informed Care
SAMHSA’s framework identifies five guiding principles that define genuinely trauma-informed practice:
- Safety — The physical and emotional environment is actively designed to feel safe. The client’s comfort is never sacrificed for clinical efficiency.
- Trustworthiness & Transparency — The clinician is honest about what is happening and why. No surprises. No hidden agendas.
- Choice — The client is always given options and maintains control over their own healing process.
- Collaboration — The therapeutic relationship is a partnership. The clinician does not “do recovery to” the client; they walk alongside them.
- Empowerment — The goal is always to build the client’s own capacity, skills, and confidence — not dependence on treatment.
How Trauma-Informed Care Differs from Traditional Therapy
The difference is not subtle. Here is how these two approaches compare across the dimensions that matter most to a trauma survivor:
| Dimension | Traditional Therapy | Trauma-Informed Care |
|---|---|---|
| Focus | Symptom or diagnosis | Root trauma & nervous system |
| Client role | Passive recipient | Active collaborator |
| Session pace | Clinician-led | Client-led, safety-first |
| Body awareness | Rarely addressed | Central to treatment |
| Goal | Manage symptoms | Restore safety & empowerment |
7 Powerful Signs You May Need Trauma-Informed Care
Trauma is not always loud. It doesn’t always look like flashbacks or visible distress. More often, it looks like exhaustion that never lifts, relationships that always seem to break in the same places, or a persistent feeling that you are somehow too much — and yet never enough.
If any of the following signs feel uncomfortably familiar, you are not alone, and you are not without options. Trauma-informed care exists precisely for what you have been carrying.

Sign 1 — You Feel Constantly On Edge or Easily Startled
What Hypervigilance Really Feels Like
Hypervigilance is not simply being “anxious” or “high-strung.” It is your nervous system operating in a permanent state of threat detection — scanning every room you enter, reading every tone of voice for danger, flinching at sounds other people don’t even notice.
This is not a personality flaw. This is a nervous system that learned, through real experience, that danger can arrive without warning. The brain adapted brilliantly. The problem is that it never got the signal to stand down.
Research from the American Psychological Association links hypervigilance directly to post-traumatic stress disorder (PTSD) and complex PTSD (C-PTSD), with the nervous system essentially locked in a fight-or-flight loop even in the absence of actual threat.
Why “Just Calm Down” Doesn’t Work — And What Does
Telling a hypervigilant person to simply relax is like telling someone with a broken leg to walk it off. The dysregulation is physiological, not a matter of will or mindset.
Trauma-informed care addresses this at the level of the nervous system — using approaches like somatic therapy, polyvagal-informed techniques, and grounding practices to teach the body, not just the mind, that it is now safe. This is why trauma-informed work so often succeeds where standard talk therapy alone does not.
Sign 2 — Emotional Numbness or Feeling Disconnected from Your Life
Understanding Dissociation and Emotional Shutdown
You go through the motions. You show up to work, have conversations, smile when it seems appropriate. But inside, there is a glass wall between you and everything you are experiencing. Life feels like something you are watching, not living.
This is not depression in the conventional sense. This is dissociation — one of the most common and least-discussed responses to overwhelming trauma. When an experience is too painful or terrifying to process, the mind creates distance. It is a remarkable act of self-protection. And like hypervigilance, it is a survival response, not a failure.
The National Institute of Mental Health recognizes dissociative responses as a direct consequence of trauma exposure, particularly repeated or early-life trauma.
How Trauma-Informed Care Helps You Feel Safe Enough to Feel Again
Effective trauma-informed treatment never forces a client back into emotional contact before they are ready. Instead, it works within what trauma therapists call the “window of tolerance” — gradually expanding a person’s capacity to feel without being overwhelmed.
Using paced, titrated approaches, a skilled trauma-informed clinician helps the nervous system relearn that emotions are survivable. Healing is not about becoming emotional — it is about becoming present again, in your own life, at your own pace.
Sign 3 — You Avoid People, Places, or Situations Without Knowing Why
Trauma Avoidance Is Not a Personality Trait
You’ve stopped going to certain places. You take a different route to avoid driving past a particular street. Large gatherings feel unbearable, not just uncomfortable. You’ve been called “antisocial” or “difficult” — but the truth is that your avoidance has a map, and that map was drawn by trauma.
Trauma avoidance is the brain’s way of protecting you from anything that resembles the original source of pain — even when the danger is no longer real. Specific smells, sounds, times of year, types of people, or even particular words can activate a full-scale trauma response long before the conscious mind registers why.
This is not irrational behavior. It is a deeply intelligent, if now outdated, threat-management system.
Identifying Your Triggers in a Safe Therapeutic Space
Trauma-informed care approaches triggers with curiosity instead of alarm. The goal is not to eliminate avoidance through force — it is to understand each trigger, approach it gradually and safely, and ultimately dismantle its power over your daily life.
Evidence-based modalities like EMDR (Eye Movement Desensitization and Reprocessing) and Cognitive Processing Therapy (CPT) are particularly effective for trauma avoidance — and both are offered through integrated trauma-informed practices.
Sign 4 — Sleep Disruption, Nightmares, or Intrusive Memories
When Sleep Becomes a Battleground
Sleep should be rest. For trauma survivors, it is often anything but. Nightmares that replay or distort traumatic events. Waking at 3am with a racing heart. Lying awake for hours as intrusive memories surface the moment the distractions of the day disappear.
Research consistently demonstrates a direct and powerful link between PTSD and severe sleep disturbance. The brain, unable to fully process traumatic memories during waking hours, attempts to do so at night — often with distressing results.
This is not weakness. This is an overburdened nervous system doing the only thing it knows how to do.
Evidence-Based Treatments That Target Trauma at the Source
Several trauma-specific approaches have demonstrated meaningful efficacy for sleep disruption rooted in trauma. EMDR, in particular, has a strong evidence base — with multiple peer-reviewed studies showing significant reductions in PTSD symptoms, including nightmares and intrusive memory, following treatment.
Imagery Rehearsal Therapy (IRT) is a trauma-informed approach specifically developed for chronic trauma-related nightmares, and may be incorporated as part of a broader treatment plan. For some patients, trauma-informed medication management can also meaningfully support sleep while deeper therapeutic work takes place.
Sign 5 — Unexplained Physical Symptoms — Headaches, Fatigue, Chronic Pain
The Body Keeps the Score — What That Actually Means
You have seen the doctors. The tests come back normal, or inconclusive. And yet the headaches continue. The exhaustion is bone-deep. Your back aches in a way that no amount of stretching resolves. You are not imagining it.
The body and the mind are not separate systems — they are one. Unprocessed trauma is stored not only in thought and memory, but in the fascia, the gut, the immune response, and the nervous system itself. This is not metaphor. It is neurophysiology.
Foundational trauma research has demonstrated that trauma survivors are significantly more likely to experience somatic complaints — physical symptoms with no clear medical origin — because the body holds what the mind cannot yet process. Chronic stress hormones, sustained over years, produce measurable damage to every major organ system.
Why Primary Care and Mental Health Must Work Together
This is precisely why the integrated model of care — where primary care and mental health treatment exist under the same roof, guided by the same trauma-informed philosophy — is so transformative.
At Paramount Health & Wellness in Portsmouth, our Family Nurse Practitioners and Psychiatric Mental Health Nurse Practitioners work together to treat the whole person. If your body is expressing what your mind hasn’t yet been able to say, we listen to both. [Paramount Health and Wellness services]
Sign 6 — Difficulty Trusting Others or Maintaining Relationships
How Trauma Rewires Your Attachment System
Relationships should not feel like this much work. And yet they do — because for someone whose earliest or most formative experiences taught them that closeness is dangerous, connection comes at a cost the nervous system is not willing to pay without a fight.
Trauma — particularly childhood trauma, interpersonal violence, or betrayal — directly disrupts the brain’s attachment circuitry. The result is a complicated dance of desperately wanting connection while simultaneously bracing for the inevitable hurt. This can look like pushing people away before they can leave. Staying silent to avoid conflict. Choosing partners who recreate familiar dynamics. Or simply feeling profoundly alone even in the company of people who love you.
This is not dysfunction. This is an attachment system that adapted to real danger and has not yet learned that safety is now available.
Building Trust — Starting with Your Therapist
One of the most profound elements of trauma-informed care is this: the therapeutic relationship itself is a healing experience. A skilled trauma-informed clinician does not demand trust — they earn it, slowly, consistently, and without judgment.
For many trauma survivors, the experience of being in a relationship where they are never pressured, always respected, and unconditionally safe is itself genuinely new. That experience begins to rewire the attachment system in the direction of health — and it transfers, over time, into every other relationship in your life.
Sign 7 — Past Therapy Hasn’t Worked — and You’ve Quietly Given Up
Why Traditional Therapy Can Fail Trauma Survivors
This may be the most important sign of all — and the one that deserves the most direct honesty.
If you have tried therapy and found it unhelpful, or worse, found it re-traumatizing, that experience does not mean you are beyond help. It may mean that the treatment you received was not designed for what you were actually carrying.
Standard cognitive-behavioral therapy and traditional talk therapy were developed primarily with anxiety, depression, and behavioral patterns in mind. They are effective for many conditions. But for unprocessed trauma — particularly complex or developmental trauma — asking someone to talk through their experiences without first establishing nervous system safety can do more harm than good.
Trauma survivors deserve care that was actually built for them.
What to Look for in a Trauma-Informed Clinician
Not every mental health professional has trauma-specific training, and the distinction matters enormously. When seeking trauma-informed care in Portsmouth, VA, look for a clinician who demonstrates:
- Explicit trauma-specific training (EMDR certification, CPT training, somatic therapy)
- A non-pathologizing approach — they never imply that your responses make you “crazy”
- An unwavering respect for your pace — no pressure to share more than you are ready for
- Integration of body-awareness with cognitive work — not just talking, but also grounding
These are not luxuries. They are the non-negotiables of genuinely effective trauma care.
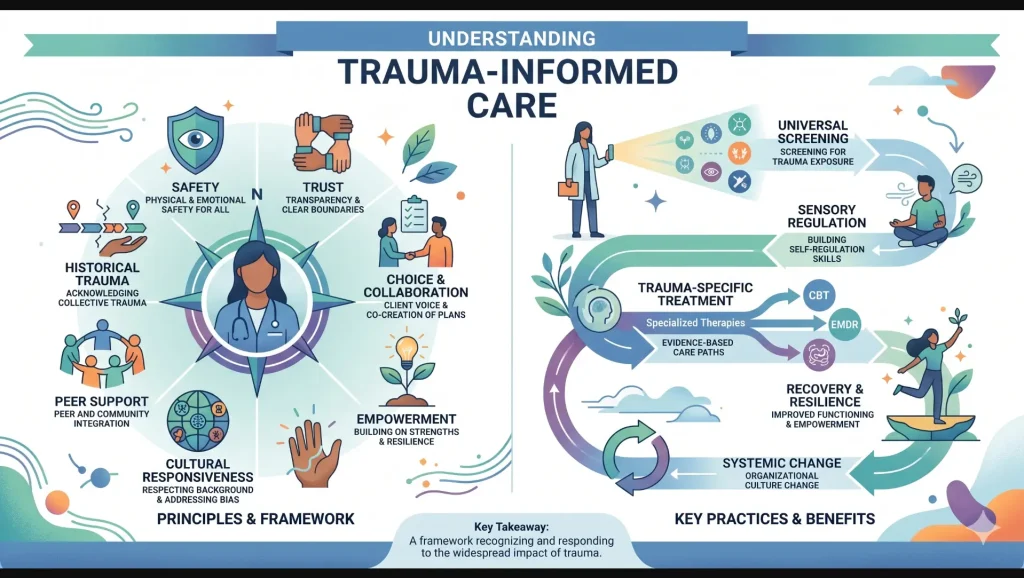
What Makes Trauma-Informed Care Different from Regular Therapy?
The question isn’t whether trauma-informed care is “better” than traditional therapy in some abstract sense. The question is whether it was built for what you need. For trauma survivors, it almost always is.
The 3 Non-Negotiables of Trauma-Informed Treatment
Regardless of the specific modality or setting, genuinely effective trauma-informed care always includes three foundational elements:
- Safety before processing — No trauma material is approached until the client has sufficient internal resources and the therapeutic relationship is stable. Rushing this stage is where trauma work causes harm.
- The therapist as collaborator, not authority — The clinician offers expertise, but the client remains the undisputed expert on their own experience. Decisions are made together.
- Whole-person treatment — The mind and body are addressed together. Physical symptoms, somatic sensations, and nervous system responses are treated as meaningful data, not background noise.
Treatment Modalities Used in Trauma-Informed Care
Several evidence-based approaches are commonly integrated within a trauma-informed framework. The right combination depends on each individual’s needs, history, and goals:
- EMDR (Eye Movement Desensitization and Reprocessing) — Strongly supported by APA and VA/DoD for PTSD. Uses bilateral stimulation to help the brain reprocess traumatic memories that are “stuck.”
- Cognitive Processing Therapy (CPT) — A structured, trauma-specific approach that helps individuals examine and shift the stuck beliefs trauma creates (“It was my fault,” “I am fundamentally unsafe”).
- Somatic Therapy — Body-centered approaches that address trauma stored in the nervous system and physical body, often essential for survivors where talk therapy alone has not been sufficient.
- Trauma-Informed Medication Management — For some individuals, medication is a valuable support alongside therapy — not a substitute for it. A PMHNP can provide both psychiatric evaluation and prescribing authority within a trauma-informed framework.
Finding Trauma-Informed Care in Portsmouth, VA
Portsmouth and the broader Hampton Roads region carry their own unique relationship with trauma. As a military-heavy community, many residents — veterans, active-duty service members, and their families — have lived with trauma that the civilian world often struggles to fully understand. Others carry the weight of adverse childhood experiences, interpersonal violence, medical trauma, or generational wounds that never had a name.
At Paramount Health & Wellness, we built our practice around the understanding that effective care must begin with that reality.
Why Portsmouth & Hampton Roads Residents Choose Paramount Health
Our integrated clinical model is specifically designed to close the gap that sends so many trauma survivors falling through the cracks of conventional care:
- Dual-trained clinical team — Our Family Nurse Practitioners (FNPs) and Psychiatric Mental Health Nurse Practitioners (PMHNPs) work in true integration, addressing physical and mental health as the inseparable system they are.
- Military and veteran-aware care — We accept Tricare and Medicare, and our providers understand the specific texture of military trauma, moral injury, and the cultural barriers that often prevent service members from seeking help.
- Telehealth across Hampton Roads — Healing should not require a long drive or lost work hours. Our telehealth services bring trauma-informed mental health care to patients throughout Hampton Roads from the privacy and safety of their own space.
- Whole-family approach — Trauma does not occur in isolation. We offer care for adults, seniors, and families — because healing one person in a family begins to heal the whole system.
What Your First Appointment Looks Like
For many trauma survivors, the hardest step is the first one. We want you to know exactly what to expect, so that fear of the unknown does not stand between you and the care you deserve:
- Your first session is a conversation, not an interrogation. You will not be asked to share more than you are ready for.
- We will ask about your current symptoms, your history, and your goals — always at your pace, always with your comfort as the priority.
- A psychiatric evaluation may be recommended to ensure you receive the most precisely tailored care.
- We will develop a personalized care plan together — which may include therapy, medication management, primary care coordination, or any combination thereof.
- Everything shared is confidential, within the standard legal and ethical parameters your provider will explain clearly.
Ready to take the first step? Book a confidential appointment with our trauma-informed care team in Portsmouth, VA. Same-day appointments available. Telehealth options across Hampton Roads. Tricare & Medicare accepted. [Book Your Appointment]
Frequently Asked Questions
What conditions does trauma-informed care treat?
Trauma-informed care is effective for PTSD, complex PTSD (C-PTSD), anxiety, depression, dissociative disorders, the long-term effects of adverse childhood experiences (ACEs), grief, and trauma related to medical events, interpersonal violence, or military service. Importantly, trauma-informed care also benefits individuals who do not carry a formal diagnosis but are experiencing recognizable trauma responses — chronic hypervigilance, emotional numbness, or relationship difficulties rooted in past experience.
Does Paramount Health & Wellness accept Tricare or Medicare for mental health?
Paramount Health & Wellness accepts Tricare and Medicare for mental health services in Portsmouth, VA. We understand the unique needs of military members, veterans, and their families across Hampton Roads. Please contact our office directly to confirm current coverage details for your specific plan. [VERIFY: confirm current Tricare/Medicare acceptance with admin before publishing]
Is telehealth trauma-informed care effective for Hampton Roads residents?
Research strongly supports the effectiveness of telehealth for mental health treatment, including trauma-focused therapy. A 2021 study published in JMIR Mental Health found that telehealth mental health services produced outcomes comparable to in-person care for PTSD and trauma-related conditions. For many patients — particularly those with demanding schedules or transportation barriers — telehealth is not a compromise. It is the most accessible and effective option available.
How long does trauma-informed therapy typically take?
Treatment length varies depending on trauma type, complexity, and individual goals. For focused, single-incident trauma, many clients experience meaningful improvement within 8 to 20 sessions using evidence-based approaches like EMDR or CPT. Complex or developmental trauma typically benefits from longer-term therapeutic relationships. Many clients report noticeable shifts in daily functioning well before the completion of their full treatment plan.
What’s the difference between a trauma-informed therapist and a PMHNP?
A Psychiatric Mental Health Nurse Practitioner (PMHNP) holds advanced clinical training in both psychotherapy and psychiatric medication management — meaning they can provide therapy and, when appropriate, prescribe medications within a single, integrated relationship. A licensed therapist or counselor typically provides therapy only and cannot prescribe. For trauma survivors whose symptoms are significantly impacting daily functioning, the PMHNP model — particularly within an integrated primary care setting like Paramount — often provides the most comprehensive path to recovery.
You Don’t Have to Carry This Alone — Healing Is Possible in Portsmouth, VA
Trauma has a way of convincing you that what you are experiencing is permanent — that the hypervigilance, the numbness, the exhaustion, the fractured relationships are simply who you are now. That is one of trauma’s most powerful and most devastating lies.
These are not character traits. They are symptoms. And symptoms respond to the right treatment.
If even one of the seven signs in this article felt uncomfortably familiar, that recognition is not a reason for alarm. It is a reason for hope. Because naming what is happening is the first step toward changing it — and changing it is absolutely possible, with the right support.
Key Takeaways:
- Trauma responses — hypervigilance, numbness, avoidance, relationship difficulty — are not personality flaws. They are the nervous system’s intelligent adaptations to overwhelming experience.
- Trauma-informed care is fundamentally different from standard therapy. It treats the root — the nervous system, the body, the attachment system — not only the surface symptoms.
- Past therapy not working is not evidence that you are beyond help. It is often evidence that the care was not designed for what you were carrying.
- Paramount Health & Wellness offers integrated, trauma-informed care in Portsmouth, VA — serving the entire Hampton Roads region in-person and via telehealth.
Ready to Begin?
Book a confidential appointment with our trauma-informed care team in Portsmouth, VA. Same-day appointments available · Telehealth options across Hampton Roads · Tricare & Medicare accepted
Book Your Appointment and Learn About Our Mental Health Services

